Application effectiveness analysis of diversified teaching combined with virtual simulation experiments in standardized training for orthopedic residents | BMC Medical Education

Mastering rapidly evolving orthopaedic surgical techniques requires a lengthy period of training. Current work-hour restrictions and cost pressures force trainees to face the challenge of acquiring more complex surgical skills in a shorter amount of time [1]. Standardized residency training (hereinafter referred to as “residency training”) is the critical bridge for orthopedic residents transitioning from theory to practice, and an essential pathway for them to grow into qualified clinicians. Traditional clinical teaching often focuses on theoretical knowledge indoctrination and basic operational skills training, while neglecting comprehensive cultivation of clinical practice skills, self-directed learning abilities, and professionalism. This single-faceted approach – characterized by “rote learning” and passive knowledge acquisition – lacks innovation and interactivity, failing to meet the demands of enhancing residency training quality. Additionally, ethical constraints and patient privacy concerns limit residents’ practical exposure to real cases, posing unprecedented challenges to clinical medical education.
The principle of current medical education is continuous participation, improvement and innovation [2]. The application of virtual simulation technology offers an effective solution to alleviate teaching pressures and serves as a vital link between medical theory and clinical practice. Integrating diversified teaching methods with virtual simulation has driven the transformation of clinical teaching models from the traditional “unidirectional” approach to a multidimensional and holistic system, providing a novel educational framework for training clinically competent physicians.
This paper aims to explore the application efficacy of virtual simulation technology in orthopedic residency training and examine how innovative teaching methods can enhance residents’ professional skills and comprehensive competencies, enabling them to meet future challenges in the medical field (Fig. 1).
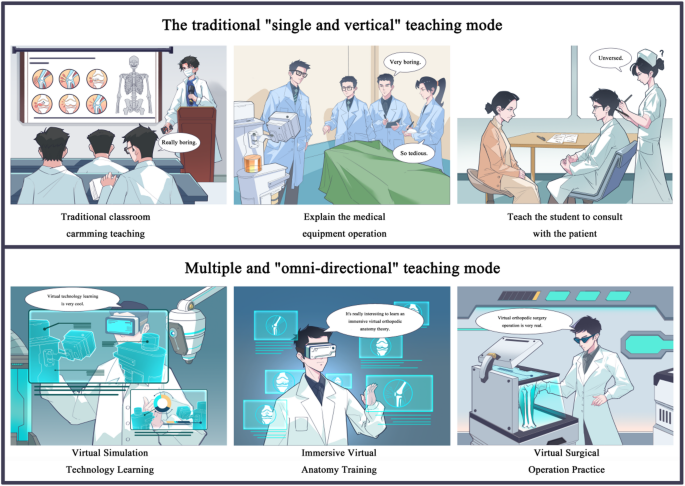
Additional teaching models: ‘single vertical’ and ‘diversified comprehensive’
Dilemmas in orthopedic residency standardization
The dilemma faced by the orthopaedic regulation and training In the global scope, especially in China, the modernization of the regulation training is a huge challenge [3], the challenge is not only limited to the technical level, but also involves the education system, resource allocation, professionalism training and other dimensions.
Technology and resource challenges
With the rapid development of medical technology, orthopedic regulation needs to integrate new technologies with The Times. Surgical skills laboratories and simulation techniques are considered important components of routine training, but the lack of funding remains a major obstacle to the development of training tools [4]. Sarah B Hays et al. in 2024 showed that robotic surgery training through a virtual reality (VR) simulator can significantly improve the surgical skills of surgical residents [4]. Despite the great potential of VR in orthopedic surgery training, its widespread application still requires further validation of [5]. Mary E Klingensmith et al. made a recommendation to review and improve the objectives, structure and funding of surgical training, indicating that multiple factors need to be considered in the technology integration process [6].
Professionalism and education system challenges
Fostering professionalism presents significant challenges due to variations across cultures and educational systems. LaPorte et al. identified erosion of professionalism as a critical issue in orthopaedic education, potentially associated with duty hour restrictions and intergenerational differences [7]. Margaret Sundel et al. further observed higher attrition rates among general surgery residents compared to other surgical specialties [8], suggesting correlations with professional development opportunities and clinical exposure. Additionally, Al-Mohrej et al. documented deficiencies in Saudi orthopedic residents’ research engagement and critical appraisal skills, highlighting training gaps in scientific literacy [9].
Modernization and personalization of educational methods
In a systematic review, Mao et al. emphasized the effectiveness of immersive virtual reality simulators in surgical training [10]. Hill et al.’s study pointed out that the number of resident physicians voluntarily participating in simulation training is limited [11], and there is a need to explore more effective incentives for training participation [12]. Bartlett et al.’s literature search revealed that further research is needed on the effectiveness and cost-efficiency of realistic simulations in orthopedic surgery training [13].
Simulation-Based Training (SBT) is a transformative method in medical education that enhances healthcare professionals’ learning and clinical skills by providing a safe environment to practice, including high-fidelity mannequins, virtual reality, standardized patients, and hybrid simulations [14]. SBT implementation faces challenges like high costs, specialized equipment needs, faculty training requirements, concerns about simulation realism, and skill transferability to real clinical settings, but future advancements, such as artificial intelligence and enhanced virtual reality, promise to increase SBT’s efficacy and accessibility [14].
Studies have shown that although surgical simulation has a role in orthopaedic training, voluntary simulator use is sporadic, resulting in many residents not receiving the full educational benefits of such training. Implementation of a mandated simulation training curriculum is desired by residents and could improve the educational return of surgical simulators in residency training [11]. That may be due to the consideration of training cost.
Role value misalignment and deficiency in humanistic care
Kalun et al. noted that residents are often seen as a “workforce” to perform daily medical tasks rather than fully educated residents, and that deviations in role values lead to dissatisfaction with professional growth. The lack of necessary humanistic care and psychological support in the high-pressure environment affected the training effect [15]. Mitchell et al. proposed that by establishing effective communication channels and actively responding to resident feedback, residents can ensure high-quality training in both professional and humanistic care [16,17,18].
Residency training challenges: an international perspective
In an international perspective, the challenges of orthopedic regulation show diversity. Pucchio et al. explored the use of AI in medical education, highlighting the importance of using and interpreting AI skills in a healthcare setting [19]. However, in China, the difficulties encountered by radiation oncology residents in the standardized training of gynecological oncology [20]. It suggests that we need to strengthen the teaching awareness of specialized trainees, and optimize the curriculum setting. Studies have shown that different countries and regions have different needs and challenges in their regulation and training.
Integrated teaching model: medical manikin and virtual simulation experiments
To meet the challenges of clinical teaching, an innovative diversified teaching and virtual simulation experimental teaching mode is implemented. This mode is based on the resident as the center, starts from the clinical learning needs of residents, supported by Medical Manikin and virtual simulation technology, to continuously improve the participation of residents, and investigate the training effect and evaluation after the training, timely improve the training system, and finally realize the improvement of residents’ clinical ability.
With the development of medical education technology, new teaching methods such as simulated surgery training system and micro class have been gradually introduced into residential training. The application of diversified teaching mode in the residential training of radiation oncology department has achieved remarkable results and provided new ideas for the teaching reform of other disciplines.
Teaching model framework
In the standardized training of orthopedic resident doctors, the diversified teaching mode of online preview, offline theory deepening, virtual simulation technology explanation, simulation case analysis and practical operation, and then the teaching effect is ensured through the five-dimensional assessment system, aiming to comprehensively improve the professional theoretical knowledge and clinical practice skills of resident doctors. The specific teaching mode is as follows:
Theoretical instruction
Theoretical teaching adopts the combination of online and offline methods, including preview from the front line of the class, offline training in the class, and online review and assessment after class, forming a set of theoretical teaching process (Fig. 2 theoretical teaching model).
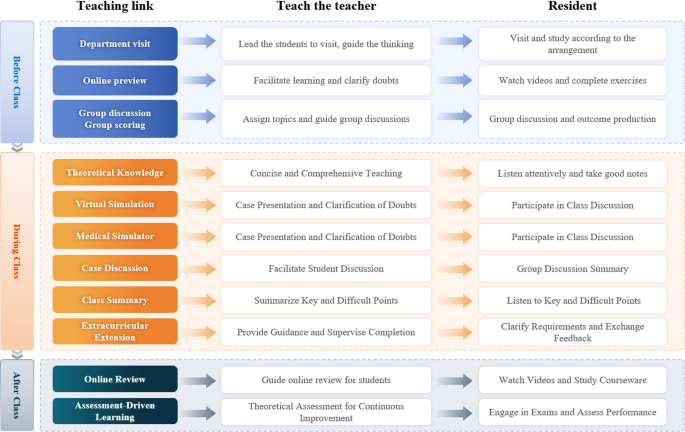
Theoretical teaching process
Online preview: Through established online platforms such as experimental space and MOOC, residents are provided with basic knowledge preview of lumbar spinal stenosis, covering disease definition, etiology, clinical symptoms and treatment strategies.
Offline deepening: A senior physician leads 3 h of offline theoretical teaching, with 1 h dedicated to the pathology, diagnostic criteria, and treatment options for lumbar spinal stenosis, 1 h on the explanation of virtual simulation technology, demonstrating to resident physicians how to use virtual reality technology to simulate the surgical process of lumbar spinal stenosis. 1 h on the case study of Medical Manikin, showing resident physicians the application of highly realistic Medical Manikin models in the surgery of lumbar spinal stenosis.
Practical training
Virtual simulation training: 1 class hour of virtual simulation training, using virtual reality technology to simulate the surgical process of lumbar spinal stenosis, including surgical step simulation, surgical skill practice and risk management.
Medical Manikin training: 1 h of Medical Manikin, using high simulation model, focusing on improving clinical operation skills, such as surgical approach, device operation and suture technology.
Five-dimensional competency evaluation
Performance theory, theory and practice results each 100 points, is divided into five dimensions (Fig. 3 five dimensions evaluation model), theory assessment from the front test (20), classroom interaction (10) and after-school test (70) two dimensions, practice assessment from solid assessment (50), experimental report (50) two dimensions.
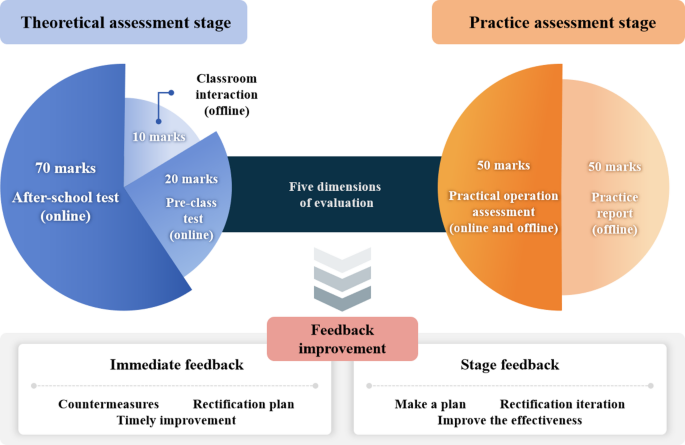
Five-Dimensional evaluation model
Teaching effectiveness
Objects and methods
Research object
Thirty residents from the Third Affiliated Hospital of Peking University were selected and randomly divided into three groups: virtual simulation group, Medical Manikin Group and Virtual Simulation Joint Human Simulation Group, 10 people in each group.
As a pilot study exploring the efficacy of combined virtual simulation and simulated patient training, the sample size was determined by pragmatic constraints: The maximum number of eligible orthopedic residents available for recruitment within the study period at our institution, and the carrying capacity of existing educational resources (e.g., VR equipment availability, simulated manikin inventory, and faculty support). This cohort size was selected to preliminarily assess trends in educational outcomes and trainee feedback. We acknowledge that the relatively small sample size constitutes a significant limitation, it may reduce statistical power, increasing the risk of Type II error, or restricts the generalizability of findings to broader resident populations. Future large-scale studies are warranted to validate these preliminary results.
Research method
Associate professors and above with rich teaching and clinical experience are serve as teachers to ensure that 30 participants can fully master the relevant knowledge and skills of lumbar spinal stenosis. Training is divided into theoretical teaching and practical operation teaching. The specific contents are as follows: ① All participants first preview through the online platform, and exposed to the basic knowledge of lumbar spinal stenosis, including disease definition, etiology, clinical symptoms and treatment strategies. The online preview platform provides rich resources, including electronic textbooks, online lectures, and interactive learning modules, which are designed to promote autonomous learning for residents. Subsequently, the participants received 3 credit hours of offline theoretical teaching led by senior physicians to deeply explore the pathophysiology, diagnostic criteria and treatment options of the condition. The teaching method adopts teaching, case analysis and group discussion to strengthen the in-depth understanding and application of theoretical knowledge.② The practical operation teaching was divided into three groups (Fig. 4 Practical training and evaluation framework): Virtual simulation group: Participants conducted 2 class hours of virtual simulation training, and used virtual reality technology to simulate the surgical process of lumbar spinal stenosis. The training content covered surgical step simulation, surgical skills exercises, and risk management, allowing participants to hone surgical skills in a safe virtual environment. Medical Manikin Group: Participants underwent 2 h of training using high-fidelity medical manikins—anatomically accurate physical models that simulate human tissue properties and allow hands-on practice of surgical techniques. These manikins provide tactile feedback and replicate real-life operative scenarios without patient risk. Virtual Simulation Joint Human Simulation Group: combining the advantages of virtual simulation and Medical Manikin training, participants have received 1 h of virtual simulation and 1 h of simulation training, and the operation experience obtained in the virtual environment can be consolidated and improved in the physical model.
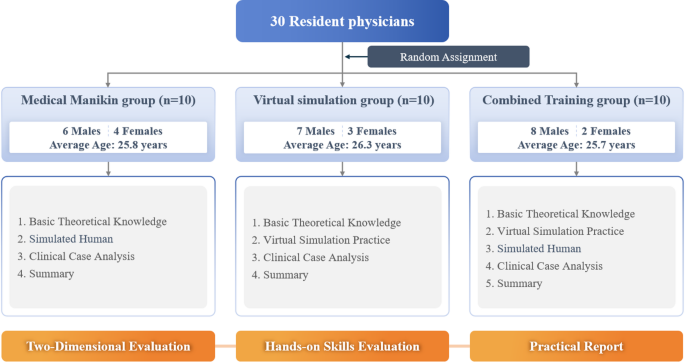
Assessment framework of practical training
Teaching evaluation
After the training, the three groups of residents were assessed in the form of examination papers. Theoretical assessment, practical operation assessment each 100 points. The theoretical assessment results and practical operation assessment results of the three groups of residents were counted separately, and statistical comparisons were made. The study utilized a questionnaire specifically developed for this research to collect data (Appendix A), for three groups of residents, the survey includes the training to stimulate learning enthusiasm, improve the learning efficiency, the effectiveness of teaching methods, training content satisfaction, cultivate the role of clinical thinking, let the resident combined with their own situation of the above several aspects, each aspect of the lowest is divided into 1 points, the highest divided into 5 points, respectively said “very dissatisfied”, “dissatisfied”, “general”, “satisfied”, “very satisfied”, finally participants questionnaire scores for statistical analysis.
Statistical methods
Statistical analysis was performed using SPSS software (version 25.0). Continuous variables that were normally distributed, as confirmed by normality tests, were presented as mean ± standard deviation \(\left(\overline{\mathrm X}\underline+\mathrm S\right)\). Intergroup comparisons for these variables were made using the independent samples t-test, which required homogeneity of variance; otherwise, the corrected t-test was applied. Categorical variables were expressed as frequency. Intergroup comparisons for categorical variables were assessed using the χ2 test, or Fisher’s exact test when the assumption regarding expected cell frequencies was not met. For continuous variables with significant intergroup differences in ANOVA, post hoc pairwise comparisons were performed using Tukey’s Honestly Significant Difference (HSD) test to identify specific group differences. A P-value < 0.05 was considered statistically significant.
link







