The study was conducted in the simulation rooms located the Teaching Facility at the Health Sciences Campus of the University of Murcia. The research was approved by the Ethics Committee of the University of Murcia (ID: 3554/2021). Informed consent to participate was obtained from all of the participants in the study.
Study sample
A total of 64 fifth-year Dentistry students from the University of Murcia—38 from the 2020/2021 cohort and 26 from the 2021/2022 cohort—carried out practical sessions using a high-fidelity simulators, the SimMan Essential simulator (Laerdal, Stavanger, Norway) (Fig. 1), as well as standardized patients. The study was conducted within the Special Needs Dentistry course and the Gerodontology course at the University of Murcia.
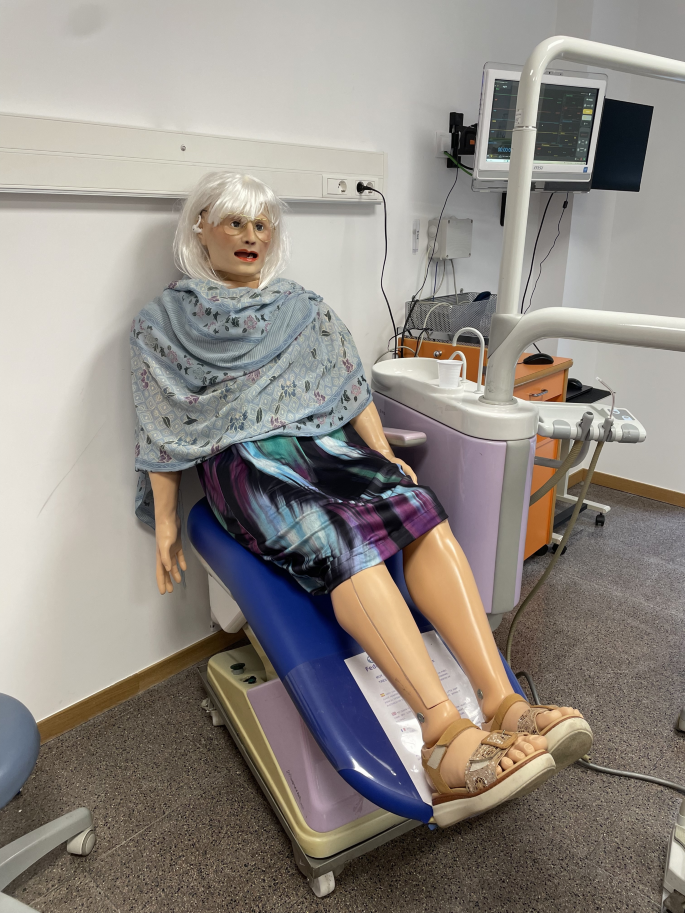
High-fidelity adult simulators used in dental education.The SimMan Essential simulator (Laerdal, Stavanger, Norway)
Inclusion and exclusion criteria
The inclusion criteria were: students enrolled in the subject Special Needs Dentistry and Gerodontology during the academic year and students who gave their authorization to be recorded for educational purposes. The exclusion criteria were students enrolled in only one of the subjects (Special Needs Dentistry or Gerodontology), and students who had already completed either of the two subjects, students who did not give their consent to be recorded for educational purposes. The activities carried out were assessed as part of the course, but only those students who agreed to participate in the study were included in the research.
Methodology
A total of six different clinical simulation scenarios were designed and implemented, each focusing on the management of medically compromised patients in a dental setting. Of these six scenarios, four involved the occurrence of a medical emergency during the dental appointment, requiring the students to respond promptly and appropriately within the clinical environment. The characteristics of each scenario—including the clinical focus, learning outcomes, simulation modality, and whether a simulated companion was present—are detailed in Table 1.
All students, in teams of 2–3, participated randomly in 1 or 2 simulation scenarios as part of the Special Care Patients course, and six months later, these scenarios were repeated and re-evaluated during the Gerodontology course, which shares content and instructors.
The methodology followed for each of the simulation scenarios was as follows:
Prebriefing
Before the simulation day, a prebriefing session is conducted to introduce students to the principles of clinical simulation and prepare them emotionally and cognitively for the activity. This phase is essential for establishing psychological safety, clarifying expectations, and fostering a respectful and collaborative environment. Instructors explain the structure, objectives, and educational value of simulation-based learning, as well as the roles that students will assume during the sessions.During this session, students are also organized into subgroups and each team is assigned one of the clinical scenarios. They receive a scenario checklist that serves as the basis for preparing their scientific report. Each subgroup is responsible for researching the assigned clinical context and developing a scientific evidence report. While there is no page limit, the document must include up-to-date references, with each team member contributing at least two properly cited sources [18, 19].
Safe environment activity
Each simulation session begins with a safe environment activity in which both instructors and students participate to promote trust, emotional safety, and group cohesion. These activities may include icebreaker games such as “Simon says,” or inviting students to share light personal facts, like what they enjoy for breakfast. The aim is to reduce anxiety, enhance communication, and create a supportive space for experiential learning [19, 20].
Briefing
Immediately before the simulation scenario begins, a briefing is conducted. Students who have prepared the scientific evidence present a concise summary of the clinical case to the rest of the group. This includes a review of the patient’s background, relevant clinical details, and anticipated challenges. The goal of the briefing is to ensure that all participants understand the scenario’s context, align on objectives, and are mentally prepared to engage in the simulation with clarity and confidence [21, 22].
Before entering the simulation room, students were informed that they would be attending to a patient returning for a second dental visit. The initial clinical history, dental examination, radiographs, and interconsultations had already been completed during the first visit. Although students had not seen this information beforehand, they were expected to simulate requesting it, and it would then appear on the monitor inside the simulation room. Their main task was to review the available data and prioritize the most appropriate dental treatment to initiate at this second appointment. Some clinical details were intentionally withheld so that students would actively ask the simulated patient and/or accompanying person, encouraging realistic communication and clinical reasoning—just as in a real consultation [21].
Simulation Scenario
A team of 2 or 3 students enters the simulation room equipped with a dental chair and all necessary instruments to replicate a real clinical setting. The room is connected to the control room through a one-way mirror, allowing instructors to observe the simulation in real time without interfering with the scenario (Fig. 2), while the rest of the group remains in the debriefing room, where they can observe the entire simulation in real time through a video feed. Within the simulation team, roles are distributed to reflect a real clinical setting: one student acts as the dentist, another as the dental assistant, and, when applicable, a third student as the circulating assistant or second auxiliary.
Dental simulation room connected to the control room through a one-way mirror
Before the simulation scenario begins, the student team is given approximately five minutes to familiarize themselves with the environment, review the available equipment, and organize the materials they may need. Then, the scenarios typically last between 10 and 15 min.
In the four scenarios that included a medical emergency, the critical event was programmed to occur at a specific point during the students’ clinical interaction—usually after reviewing the patient’s history or initiating treatment. The emergency (e.g., hypertensive crisis, hypoglycemia, asthma attack, epileptic seizure) was simulated through changes in the high-fidelity mannequin’s vital signs (e.g., blood pressure drop, respiratory distress, seizure activity) or verbal cues provided by standardized patients or instructors from the control room. Students were expected to recognize early warning signs, communicate effectively, and implement appropriate clinical protocols (e.g., positioning, oxygen administration, use of emergency kit, activation of emergency services). Instructors adjusted the scenario dynamically based on the students’ actions to maintain realism and ensure educational objectives were met.
Throughout the simulation, instructors are located in the control room (Fig. 3), where they manage the physiological parameters of the simulator and/or standardized patient, provide verbal responses when necessary, and observe student performance.
Control room where instructors monitor and manage the simulation in real time
-
Evaluation is carried out in real time using standardized checklists designed by the research team for each simulation scenario. These checklists included both technical and non-technical competencies such as decision-making, teamwork, communication, and prioritization of care. The content of the assessment checklists was validated by an expert panel composed of 11 faculty members from six Spanish universities, all of whom are professors of the Special Care Dentistry course in their respective institutions, with a minimum of 10 years of clinical and teaching experience in this field. The experts independently reviewed each item using Likert-type scales to assess its importance and relevance for the evaluation of the scenarios. The checklists were then refined through a consensus process and piloted in prior simulation sessions before formal use in the study.
Debriefing
After the scenario ends, the participating students and the instructors return to the debriefing room. First, the students who performed the simulation share with the group how they felt, and then a guided and collective discussion begins to evaluate and reflect on the positive aspects and areas for improvement in the scenario they experienced.
In addition to the simulation itself, the methodology incorporated structured group learning and peer feedback components. During each session, while one team performed the simulation, the remaining students observed the scenario in real-time from the debriefing room. These students were encouraged to identify and record both effective actions and areas needing improvement. This process fostered collaborative reflection and discussion during the debriefing phase, where students collectively evaluated the scenario and exchanged perspectives. This approach enabled not only experiential learning but also peer-supported development of clinical and communication skills.
Evaluation
Evaluation of the students was carried out using the previously described assessment checklists. These checklists were completed twice: the first time during the subject Special Needs Dentistry, and a second time six months later, during the repetition of the clinical scenarios in the subject Gerodontology. All scenarios were recorded with the aim of using the recordings, if necessary, to improve the accuracy of the evaluation and during the debriefing session.
After collecting all evaluations from the three instructors, the results were compiled into Excel spreadsheets—one for each clinical scenario. The data were collected item by item, recording the evaluation provided (Yes/No) by the three evaluators in the initial simulation (PRE) and six months later (POST).
Data analysis
All the initial and final evaluation results of the students, obtained through the assessment checklists, were sent to the Statistical Support Section (SAE) of the University of Murcia. Data analysis was performed using R version 4.0.3. Normality and homoscedasticity (equality of variances) between the scores given by each observer in the initial and final evaluation of each assessment checklist were analyzed. For this purpose, Bartlett’s test and one-way ANOVA were used. Additionally, an average score per student was calculated based on the evaluations given by the three assessors for each checklist in both the initial and final assessments, and the p-value was calculated to determine the presence or absence of normality. Subsequently, either a paired t-test or a non-parametric paired test (if normality was not present) was used to determine whether the results were statistically significant.
link

