Implementation of United Arab Emirates competency framework for medical education in undergraduate medical curriculum | BMC Medical Education

To ensure consistency with national educational standards, the UCFME thematic roles were systematically mapped to the QF-E. This ensures that the development of medical professionals adheres to educational benchmarks established for various qualification levels within the UAE. This mapping, illustrated in Table 3, bridges the competencies outlined in UCFME with the levels, descriptors, and outcomes specified in the QF-E [21, 30].
The mapping of PLOs and CLOs with UCFME themes, illustrated in Figure 3, demonstrates how the RAKCOMS MD Program achieves constructive alignment. The schematic flow diagram visually represents the interconnectedness of UCFME themes, PLOs, and CLOs within the RAKCOMS MD Program. It highlights the logical progression from the UCFME framework to program-level outcomes, course-level outcomes, and instructional design. The diagram serves as a blueprint for curriculum developers and faculty to maintain alignment and coherence in the educational process [21].
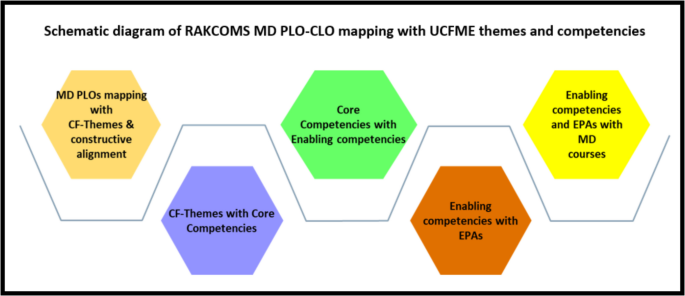
Schematic diagram demonstrating RAKCOMS MD PLO-CLO mapping with UCFME themes and competencies
The mapping of RAKCOMS MD Program Learning Outcomes (PLOs) with the UCFME themes, as shown in Table No-4, ensures that the program’s educational goals align with the competencies required for professional medical practice, identifies gaps or redundancies in the curriculum and facilitates alignment between learning outcomes, teaching strategies, and assessment methods [21, 26, 30].
Mapping of UCFME Themes, core competencies, enabling competencies and EPAs are done for each course according to the format table shown below (Table No-5).
The EPAs are designed to encapsulate the practical application of competencies in real-world clinical settings. To streamline curriculum design and ensure targeted learning, the EPAs are categorized as follows:
-
Essential (E): These EPAs are critical and foundational for all medical graduates. They represent tasks and responsibilities that every graduate, regardless of future specialization, must be proficient in to ensure safe and effective patient care.
-
Important (I): These EPAs are highly significant but may not be universally required in all clinical contexts. Proficiency in these activities may depend on the specific career path or clinical environment a graduate chooses.
-
Relevant (R): These EPAs are context-dependent and may not be directly applicable to every graduate’s practice. They are still included in the curriculum to provide a broader understanding of the professional roles and responsibilities, allowing learners to adapt to diverse medical scenarios.
Table 6 provides a detailed breakdown of the 14 EPAs into these three categories. This classification helps in Curriculum design where educators can allocate time and resources efficiently by focusing primarily on the Essential and Important EPAs while ensuring exposure to Relevant ones [22]. Also formative and summative assessments are planned based on the priority level of EPAs. It also assists students in understanding the expectations for their training and prioritizing their learning efforts accordingly.
The EPAs are integrated into the medical curriculum with incremental complexity starting from MD Year 2. This approach ensures a gradual progression in students’skills, knowledge, and responsibilities. Table 7 visually outlines how each EPA is distributed across the curriculum. RAKCOMS MD Years 1 (semester-I & II) and 2 (semester-III & IV) are called as “pre-medical” years. MD Years 3 (semester-V & VI) and 4 (semester- VII) are the “pre-clinical” years. MD Years 4 (semester-VIII), 5 (semester-IX & X) and 6 (semester-XI & XII) are designated as “clinical” years. In MD Year 2, students are introduced to the basic components of EPAs. Activities focus on foundational skills such as history taking, physical examinations, and simple clinical reasoning under close supervision. Emphasis is placed on developing a strong knowledge base and building confidence in performing routine tasks. During intermediate complexity in MD Years 3 and 4, students progress to more complex tasks that require integration of multiple skills, such as formulating differential diagnoses, interpreting diagnostic tests, and participating in patient management. Supervision levels are adjusted based on student competence, fostering independence while maintaining patient safety. Opportunities are provided for students to take on greater responsibility in clinical settings. In advanced complexity in Final Year, students are expected to demonstrate near-independent proficiency in all core EPAs. Activities may include managing acute care scenarios, performing specific procedures, or coordinating interprofessional care. The focus shifts to emphasizing decision-making, leadership, and adaptability in diverse clinical contexts.
Figure 4 serves as a visual and comprehensive summary of intended EPA achievements for each graduate by the end of the MD program. It reflects how students have progressed in each EPA, their competency milestone stages at which critical competencies will be achieved and alignment with Program Goals. The figure visually demonstrates the gradual development of EPA competencies across different MD years, showing incremental complexity and increasing levels of independence [22, 31]. It highlights how foundational skills in earlier years evolve into advanced, integrated competencies in later years.
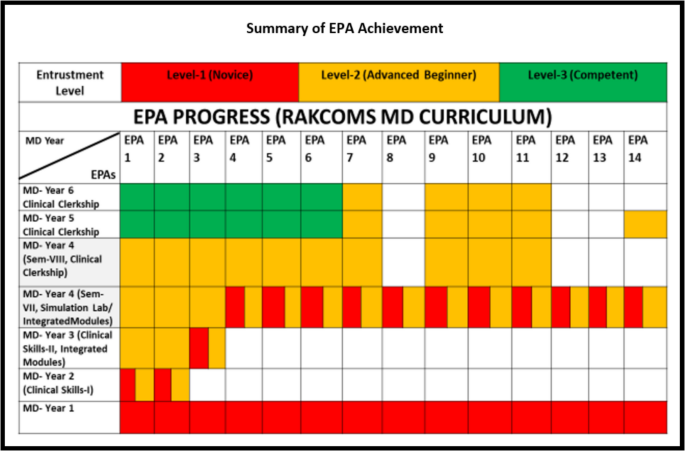
Summary of intended EPA achievements for each graduate by the end of the MD program
Assessment in the medical curriculum is a critical component of ensuring that students acquire the necessary knowledge, skills, and attitudes to become competent medical professionals. To achieve this, the RAKCOMS MD Curriculum employs a variety of assessment tools and instruments tailored to measure different domains of learning (cognitive, psychomotor, and affective). These tools are systematically illustrated in Table No-8. By this mapping, educators and students can easily understand how each domain of learning is assessed, ensuring alignment with CLOs. The use of diverse tools also ensures that all aspects of a student’s development (knowledge, skills, attitude and professionalism) are thoroughly evaluated [32,33,34]. Mapping tools to curriculum objectives helps identify any gaps or redundancies in the assessment process, allowing continuous improvement [35,36,37].
EPA Observation Checklist is a tool used to document and assess the performance of medical students or other trainees in specific professional activities. The checklist serves as a structured way to observe and evaluate these activities in real-time during clinical encounters, providing valuable feedback for both students and instructors. The checklist includes specific EPAs where each EPA is clearly defined (e.g., taking a patient history, performing a physical exam, or managing a clinical situation) so that students know what is expected of them. It also includes specific behaviors and performance indicators that need to be observed to assess the student’s competency in performing the activity. The checklist also includes different levels of supervision, from direct observation to independent practice, depending on the student’s progress and there is a feedback section to provide feedback, highlighting strengths, areas for improvement, and specific suggestions for development (Figure 5) [35, 37].

EPA Observation checklist to document and assess the performance of medical students or other trainees in specific professional activities
The “Priority Index” in evaluation is a framework used to prioritize which EPAs should be evaluated with more focus during a student’s training [38]. This helps in identifying key areas where students may need more attention and guidance, ensuring that assessments are aligned with the most critical learning objectives at a given stage of their education. In Table No-9, the Evaluation Priority Index is visually represented to show how different EPAs can be ranked according to their significance at each stage of training. In Table No-10, the EPA-Competency Domain Evaluation Matrix visually organizes how each EPA is given a relative weightage with respect to the impact (EPA importance) and learner progress (milestones) for assessment. The EPA evaluation weightage is shown as radar chart in Figure No-6.

EPA evaluation weightage radar chart
Challenges and enablers
The UCFME represents a significant step in advancing medical education in the UAE. It aligns with international standards while addressing the unique healthcare challenges and cultural context of the region. Implementing this framework, however, involves navigating various challenges and leveraging enablers to ensure its success.
Collaborative integration among medical schools required strategic coordination and alignment, initially met with logistical and cultural barriers due to institutional autonomy, varying infrastructural capacities, and differences in faculty familiarity with competency-based education principles. While faculty generally supported the initiative, resistance was evident among some educators, stemming primarily from uncertainties regarding competency-based assessment methodologies and apprehensions about increased workload and responsibilities.
Challenges in implementation
Institutional readiness- Many medical institutions may lack the infrastructure, resources, or expertise to adopt UCFME effectively. Resistance to change from faculty and administrative staff further complicates the transition [4]. In the UAE, disparities in resource allocation among institutions exacerbate this issue [40].
Faculty development- Faculty members often require training to understand and apply UCFME principles. Limited access to professional development opportunities and insufficient training in modern pedagogical methods can hinder this process [41, 42]. Research underscores the importance of faculty development in successful competency based education implementation [43, 44].
Assessment challenges- Designing and implementing competency-based assessments require significant resources and expertise. Ensuring reliability and validity while accommodating diverse learner needs poses additional challenges [34, 39, 45,46,47].
Cultural considerations The UAE’s multicultural environment necessitates a framework that respects cultural diversity while maintaining global standards. Balancing these aspects can be challenging [48].
Policy and regulatory barriers- Fragmented policies and inconsistent regulatory support can delay implementation. Coordination among stakeholders, including government bodies, accreditation agencies, and institutions, is essential [49, 50].
Enablers of implementation
Government support- The UAE government’s commitment to advancing healthcare and education serves as a strong enabler. Investments in medical education and healthcare infrastructure create a conducive environment for the framework’s implementation. Government initiatives, such as the UAE Vision 2030, emphasize education and healthcare as national priorities [51].
Existing educational excellence- Many UAE medical institutions already adhere to international accreditation standards, providing a solid foundation for integrating the UCFME [40, 52].
Technological advancements- The UAE’s investment in digital infrastructure facilitates the integration of technology-enhanced learning and assessment tools, which are essential for UCFME [40, 53].
Collaborative networks Partnerships among institutions, government bodies, and international organizations foster knowledge sharing and resource pooling [6, 40, 54].
Mitigation strategies
To enhancing institutional readiness, comprehensive needs assessments is warranted to identify gaps in infrastructure and resources. Funding and support from government and private sectors can be secured to address resource disparities which facilitates successful implementation of UCFME. It represents a unique advantage within the UAE context. Substantial financial and infrastructural support is explicitly driven by the UAE government’s strategic commitment to elevating national healthcare standards and aligning medical education with international benchmarks. However, recognizing the variability in global contexts, alternative funding strategies are recommended, including international collaborative partnerships, grants from educational foundations, and public–private collaborations, which could be viable for regions without equivalent governmental support. For faculty development, continuous professional development programs needs to be implemented focusing on CBME principles. Culturally adapted faculty development workshops are integral in overcoming initial resistance and enhancing educator competencies, addressing cultural sensitivities, language barriers, and differing pedagogical traditions effectively. These targeted interventions not only bolster faculty confidence but also strengthen stakeholder engagement, facilitating a smoother transition towards competency-based medical education. Mentorship programs to support faculty during the transition are recommended. The “Train-the-Trainer” (TTT) initiative in Canada’s CBME implementation provides a model for faculty development [4, 41, 42]. The primary difference is one of context and scale: Canada’s TTT was implemented alongside a nationwide CBME rollout in residency, whereas our effort is in undergraduate education and will be tailored to UAE’s local needs and resources. Thus, the principles (peer-led faculty development, cascade training) can be adopted with customizing the content and delivery to our environment.
In order to improve assessment strategies, standardized guidelines for competency-based assessments needs to be implemented. Investments in assessment technologies, such as e-portfolios and simulation-based evaluations are required. The use of OSCEs has been successful in competency-based assessment globally [37,38,39,40]. To address cultural considerations, diverse stakeholders in framework development need to be engaged to ensure cultural relevance. Cultural competence training for both educators and learners can be incorporated [48]. To streamline policies and regulations, fostering collaboration among regulatory bodies to create unified policies and establishing a national task force to oversee and coordinate implementation efforts are required. The ACGME model in the US demonstrates the importance of centralized oversight [50].
link







