New approaches and established models for scaling up sex- and gender-sensitive medicine teaching
Despite two decades of experience, the integration of SGSM into medical curricula still faces multiple barriers. Practitioners are often accused of introducing a political-ideological standpoint that defies the concept of medicine as ‘objective’ and ‘neutral’, undermining the status of SGSM and hindering its implementation3,25,26. A lack of best-practice examples as well as fluctuating resources in terms of funding, personnel, expertise, or time, are other barriers19,25,27,28.
To analyze the integration of SGSM into medical education, we first examined different models. Understanding these different models can provide a framework for the future integration of SGSM. Since medical curricula differ in structure depending on the local academic context, knowledge about different implementation approaches can support the adaptation of teaching formats to the local context.
Models of curricular integration
Building on the framework by Verdonk and Davis-Russel, we highlight some practical implementation examples in line with the four proposed models of integration.
-
a.
The separate-course model, which includes specific courses in sex- and gender-specific medicine.
-
b.
The area-of-concentration model provides in-depth education for interested students.
-
c.
The interdisciplinary model
-
d.
The integration model in existing courses and curricula3,29.
Separate-course model
The separate-course model consists of offering a course or lecture series about SGSM in addition to the existing medical curriculum. The thematic focus can range from general SGSM to specific topics, such as the influence of sex and gender on individual diseases. The implementation is relatively simple, as a lecture series oftentimes does not need to comply with complex implementation requirements, and the existing curriculum does not need to be changed29.
Therefore, the separate-course model is a quite popular integrational model, found amongst others at the Austrian medical faculties30, at Seoul National University College of Medicine27, or in the form of intersectionality courses at Harvard Medical School31 or the Pritzker School of Medicine, University of Chicago32.
The add-on nature of this model is also its disadvantage: it is less effective because the teaching is isolated, oftentimes offered only during one semester. This shortcoming can be partially addressed by implementing a separate-course model for SGSM during consecutive semesters33,34.
Area-of-concentration model
The area-of-concentration model focuses on working with smaller groups of interested students. It frequently takes the form of an elective, offering the students an in-depth learning experience. This may lead to a higher degree of skill acquisition and may encourage the students to pursue future research activities, such as theses and dissertations29. The elective format also enables creative didactic approaches to SGSM teaching, for example, using web-based classes or Meet the expert-formats1. However, since it only provides teaching for a small number of already interested students, it does not reach the majority of the students who will work in patient care.
The area-of-concentration model also does not require a reorganization of the curriculum, making it a popular option, for example, at Karolinska Institutet, Sweden, Medical University of Lodz, Poland, Warren Alpert Medical School of Brown University, and various Dutch faculties1,35,36,37.
Interdisciplinary model
The interdisciplinary model entails the attendance of courses allocated within or organized in collaboration with other faculties3,29. In an academic context, this model requires interdepartmental cooperation and organization but may prevent redundancy between different curricula and thus make better use of institutional resources29. This can be an advantage when limited resources are a barrier to SGSM integration. The interdisciplinary model can be combined with other integration models, such as separate courses, electives, or longitudinal integration, and can foster interdisciplinary teaching.
Another advantage of this approach is the dissemination of different perspectives, for example, between gender studies and medicine38, or within sexology, legal medicine, and other disciplines39. Interdisciplinary teaching may strengthen the knowledge of concepts of sex and gender, power and intersectionality40, or legal frameworks such as anti-discrimination law.
Integration model
Verdonk et al. describe the integration model as the most successful implementation of SGSM3. In this model, SGSM lectures and courses are incorporated across the curriculum, ideally in all semesters and with growing complexity. However, the integration model is also the most difficult option to implement: longitudinal, cross-cutting integration of SGSM requires redesigning existing curricula to accommodate the inclusion of sex and gender29,41, it is time-consuming3 and involves multiple stakeholders from different faculties.
Teaching gender-sensitive clinical skills is especially important because students report feeling insufficiently prepared to implement sex and gender-sensitive competencies into everyday clinical practice42,43. In this regard, longitudinal, competency-based integration may have a positive impact on students’ subjective feeling of preparedness44.
Faculties in Europe that integrate SGSM teaching longitudinally are Radboud Nijmegen36,39,45, the medical faculty of Innsbruck46,47,48, Ulm49, and Charité Berlin41. Comparing the programs as cited in the literature, Radboud Nijmegen, Charité Berlin, and the medical faculty of Ulm show a similar approach in offering obligatory specific SGSM courses, as well as a longitudinal cross-cutting integration in different modules of undergraduate and graduate curricula. In contrast, the faculty of Innsbruck states two obligatory lectures on SGSM in the third and ninth semesters, and further unspecified seminars. All four faculties offer additional electives in SGSM, some combined with other aspects of diversity. Due to the outdated publication dates, we consulted the relevant coordinators of SGSM teaching in each faculty to obtain an updated perspective. At Radboud Nijmegen, due to a recent restructuring of the medical curriculum, the cross-cutting SGSM implementation is currently uncertain and subject to a curricular-wide inventory. Charité Berlin, Innsbruck, and Ulm confirmed the actuality of longitudinal cross-cutting integration as reported within the cited publications. The different programs also exemplify the adaptation of the integrational model to specific faculties and contexts.
University teachers and staff
Effective implementation also relies on the capacity of university lecturers and staff to utilize and effectively promote specific educational methods. Research shows that lecturers and academic staff can endorse gender stereotypes, perceive SGSM as less important than students themselves, and perpetuate stereotypes through the hidden curriculum26,50,51.
Therefore, implementing SGSM in medical education also means strengthening the sex, gender, and diversity-related competences of lecturers and university staff. Enhancing educators’ expertise allows them to better support the implementation of SGSM in medical training, ensuring that both the teaching staff and students are adequately prepared for its integration. Boston University Medical Campus, therefore, introduced a one-session voluntary training on sex, gender, and SGSM teaching for educators, including a didactic input, a small-group session with a learning case, and a large-group discussion on how to modify teaching practices52. Similar trainings were implemented in the University of California, Davis, Medical Center, Baylor College of Medicine – The Children’s Hospital of San Antonio, Texas53, and Cambridge Health Alliance with a focus on racial and ethnic minorities and cultural identity54.
Another approach has been developed at SUNY Upstate Medical University, which implemented a bias checklist as an obligatory self-assessment tool for lecturers´ own teaching materials55. The Upstate Bias Checklist, adapted by numerous faculties across the U.S., trains lecturers in detecting, reflecting, and preventing multiple biases in education content, such as race and ethnicity, sex and gender, sexuality, disability, mental health, weight, poverty and socioeconomic status, age, religion, and many more.
University leadership
Top-down support by university leadership, such as deans and faculty managers, as well as institutional policies, is an important step toward the implementation of novel teaching approaches. In the cited examples, different structural factors appeared to support the faculties in their implementation efforts. Several initiatives recommend the involvement of e.g., “change agents” or “trigger persons” that accompany the curricular mapping and reorganization processes in the faculty21,41,45. Structural requirements for accreditation are also an institutional lever to facilitate the top-down implementation of curricular innovations. At Charité Berlin, the faculty leadership supported the implementation of novel SGSM content in the curriculum in the context of an accreditation process. For successful implementation, a change agent was hired, who developed, standardized, and monitored curricular adaptations within the departments41. Top-down support was also cited by Böckers et al. Specifically, the dean and faculty council assigned a task group to design the SGSM curriculum, which involved the lecturers of cross-cutting subjects49. Formal academic structures can also function as levers, as described by Hochleitner et al., who reported on the influence of the chancellor’s office in convincing the previously unsupportive university leadership to implement SGSM48. In addition, Verdonk et al. mention that the local Dean only supported the continuation of a curricular revision after the performance of an initial curricular mapping. The local effort eventually led to a national project45.
These examples highlight the fundamental role of leadership in fostering change, but also that successful implementation can be achieved through different approaches and that local organizational culture and structures need to be considered.
A new model for SGSM in medical education
It has been repeatedly observed that a lack of best-practice examples is a significant barrier toward implementation, even at a medium-level19. Furthermore, a lack of devoted resources, such as a change agent or a local department of SGSM, limits the applicability of recommended strategies.
Therefore, to aid the systematic evaluation of implementation efforts, we introduce a new model of integration of SGSM into medical education (Edu-GRAS), adapted from the Gender Responsive Assessment Scale (GRAS)56 (World Health Organization: Gender mainstreaming for health managers: a practical approach. Participant’s notes. (2011)). The new model defines the depth of implementation of SGSM at the curricular level. In addition to the content evaluation, we specify the profile the learner should develop at different stages and the competences acquired. The framework can be used as a strategic tool to guide implementation efforts or as an analytical framework to describe existing practices.
The GRAS was presented by the World Health Organization in 2011 to assess the implementation depth of gender equality strategies and interventions (World Health Organization: Gender mainstreaming for health managers: a practical approach. Participant’s notes. (2011)), and has been adapted and applied to multiple contexts, for example in immunization, COVID-19 response plans, female genital mutilation57,58,59,60, and medical research (Canadian Institutes of Health research: Sex/gender-responsive assessment scale for health research: (2021)); Nehem B.V.: Integration of the gender dimension into research and teaching content. (2020). Adapted to medical education, it provides operational definitions and facilitates an incremental approach to curricular change toward in-depth SGSM implementation.
The GRAS was not a direct result of the literature search, as it derives from the context of public health intervention assessments. We adapted the GRAS to the setting of medical education to structure the findings of our literature search and provide an operative assessment tool for SGSM in medical education, given the current absence of an applicable tool3.
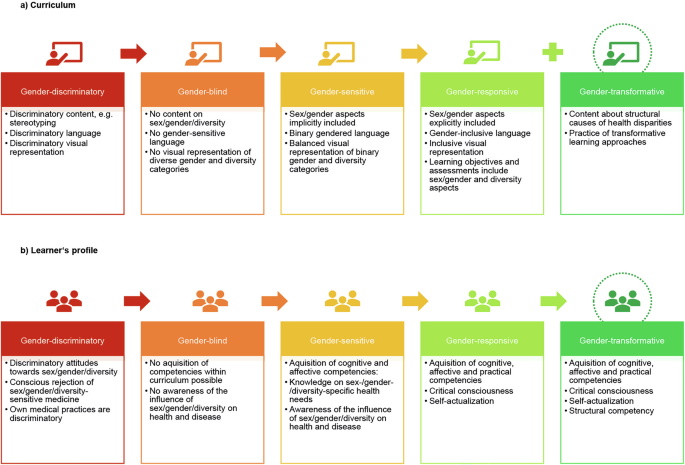
The GRAS encompasses 5 steps, ranging from gender-discriminatory to gender-transformative56 (UNFPA: Joint Evaluation of the UNFPA-UNICEF Joint Programme on the Elimination of Female Genital Mutilation: Accelerating Change Phase III (2018–2021). Gender responsive and/or transformative approaches. (2021)). In the following section, we present the individual stages and their adaptation to medical education (see Fig. 1).
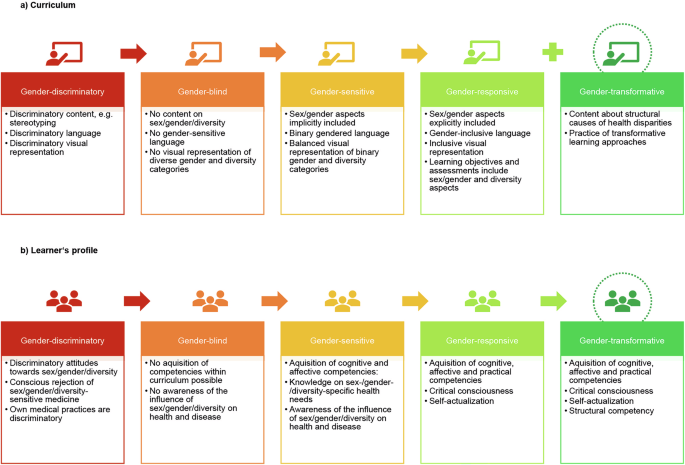
The Gender Responsive Assessment Scale adapted to medical education (Edu-GRAS) – curricular content and promoted learner´s competences. a represents sex, gender, and diversity-related content within the curriculum. The curriculum can range from gender-discriminatory to gender-transformative depending on the focus and depth of teaching materials and content (illustrated from red to green). b represents the transmitted learner’s competences. Learner´s profiles also range from gender-discriminatory to gender-transformative with increasing knowledge acquisition, engagement, and self-awareness (illustrated from red to green).
Gender-discriminatory
The first stage is a gender-discriminatory curriculum. Discrimination on the grounds of sex, gender, and diversity is embedded in medical education, if it solely employs a “white, western, cis male” as standard40,61. It directly and indirectly engenders discriminatory attitudes, through its explicitly taught content, but also through narrow linguistic and visual representation40,62,63 and other aspects of the hidden curriculum64. Therefore, a discriminatory curriculum engenders discriminatory attitudes in learners, which causes the reproduction of long-standing discriminatory medical practices.
Gender-blind
A gender-blind curriculum does not explicitly address content or representation of SGSM or diversity, however, it also does not purposefully reiterate the presence of just one standard. Therefore, it does not openly transmit discriminatory content or representation, but still reproduces bias65. The transition between a gender-discriminatory and a gender-blind curriculum is fluid, since biased representation can result in discriminatory practices. The learners cannot acquire competences nor develop awareness regarding SGSM and diversity through the curriculum, rather, they are prone to adapt biased attitudes themselves.
Gender-sensitive
A sex-, gender- and diversity-sensitive curriculum addresses sex/gender/diversity-specific needs, such as sex/gender-specific diagnostics and therapy, but fails to contextualize them66,67. An example could be the representation of sex-disaggregated mortality rates for different diseases in the absence of additional contextualization. Biological factors such as chromosomes or hormones have a crucial influence on body fat distribution, metabolism, immune response, and renal function4 – and should be addressed explicitly to provide context to the illustrated sex-specific variations in mortality. Decontextualized numerical representation of sex differences might, nevertheless, be a straightforward first implementation step since it reproduces the biomedical – oftentimes decontextualized – focus of traditional medical curricula22.
Language and visual representation are gender balanced, although in a strictly binary form. The learner can acquire cognitive competences and develop affective competences, such as gender awareness. Although mostly focused on binary description, learners acquire knowledge and understanding of gender as a social determinant of health, and are sensitized toward the negative effects of stereotypes such as “the whiny woman” or “the tough man”3,68. Gender sensitivity can be achieved through a focus on the general theoretical underpinning of sex and gender, and potential courses on gender stereotypes, prejudice, and gender awareness36,46,48.
At this level, no remedial practical competences are developed. Nevertheless, awareness is the first step toward a gender-sensitive medical practice, followed by acceptance, adoption, and adherence69. To foster gender awareness, therefore, means to provoke change.
Gender-responsive
A gender-responsive curriculum implicitly and explicitly focuses on the impact of sex/gender and diversity on health, providing depth and context66,67. It addresses specific needs, barriers to care, and access to resources in a broader context. Through a gender-responsive curriculum, learners are able to acquire cognitive competences, such as in-depth knowledge about sex/gender/diversity-specific health/disease measures, as well as affective and practical competences for gender-responsive medical care.
The sole knowledge of sex and gender-specifics does not automatically translate into better health care, as biased attitudes can remain65. Gender-responsive clinical care means challenging stereotypes and intentionally adapting one’s practice. Most practical skills taught through an SGSM-sensitive curriculum are social competences, such as gender-sensitive patient-provider communication that explicitly addresses gender roles and stereotypes, as exemplified by the medical faculty of Innsbruck or the Harvard Medical Faculty31,46. The Medical Faculty of Lausanne implemented a reflexivity course about gender biases encountered during a clinical internship in general ambulatory medicine, encouraging students to reflect on biases in clinical reasoning about real-life patients70.
In addition to contextualized content, gender- and diversity-inclusive language, as well as inclusive visual representation, are used in a gender-responsive curriculum62,63,71. This includes verbally and visually referring to patients and physicians of different genders and representing people with different skin colors and abilities, as well as avoidance of stereotyping and othering62.
Learning objectives and final assessments should include sex/gender and diversity aspects45,66. Verdonk and colleagues developed criteria and learning objectives for the successful integration of SGSM in medical curricula, which were widely adapted by other faculties35,39,41,45.
A gender-responsive curriculum also fosters critical consciousness in the learner, showcasing how medicine is embedded in broader social structures and affected by disparities72. Critical consciousness enables the learner to think contextually and take the patient´s and communities´ context into consideration73. Following a critical pedagogy approach, the University of Michigan Medical School offers a course on multicultural competencies that fosters engaged dialogue and reflection of social issues through case studies and interactive theater formats72.
To foster a gender-responsive medical practice also means to “include self-reflection on and self-awareness for one’s gender role, privilege, and power”23. Self-actualization counteracts the idea of a fixed set of competences a learner can master, but implies the understanding of SGSM competencies as a constant learning process one can only achieve over time and with constant reflection and openness to development72,73,74.
Gender-transformative
Compared to a gender-responsive curriculum, a gender-transformative curriculum explicitly addresses and, ideally, transforms the structural origins of health inequities and social disparities. It aims to change norms and power structures, addressing the roots of (health) inequalities and discrimination, and aims for transformation of the structures that create and maintain these inequalities56. A gender-transformative curriculum broadens the focus beyond medical practice and focuses on the overall social, institutional structures where the medical system is embedded.
The content and practical competences imparted are transformative themselves. This requires time, depth, and a facilitating atmosphere, oftentimes not available in medical curricula due to tight schedules, the amount of imparted cognitive content, and tight testing requirements. The required type of teaching is, therefore, challenging to provide in medical schools. In addition to the acquisition of cognitive, affective, and practical competences and the cultivation of critical consciousness and self-actualization, learners are enabled and empowered to develop structural competencies. Interactive formats, in particular, can encourage students to take action.
Metzl and Hansen propose a seminar where students are asked to design their own structural interventions. They cite, among others, Nashville Mobile Market, a student-run initiative in Tennessee, U.S., that hires refrigerated food trucks to drive to impoverished areas to enable low-income patients to take their medication after meals74.
In the field of SGSM, gender-based violence is included in some medical curricula following a transformative approach. Gender-based violence includes physical, psychological, and sexual violence and abuse (European Commission: What is gender-based violence? Gender-based violence can take different forms and mostly affects women and girls. (2021)), and should be taught with a trauma-informed pedagogy75. The faculty of Lausanne teaches a prevention-based approach to sexism and sexual harassment in a compulsory interactive theatre format, which explicitly functions as corrective education33.
link





