The impact of sensory integration based sports training on motor and social skill development in children with autism spectrum disorder
Research design
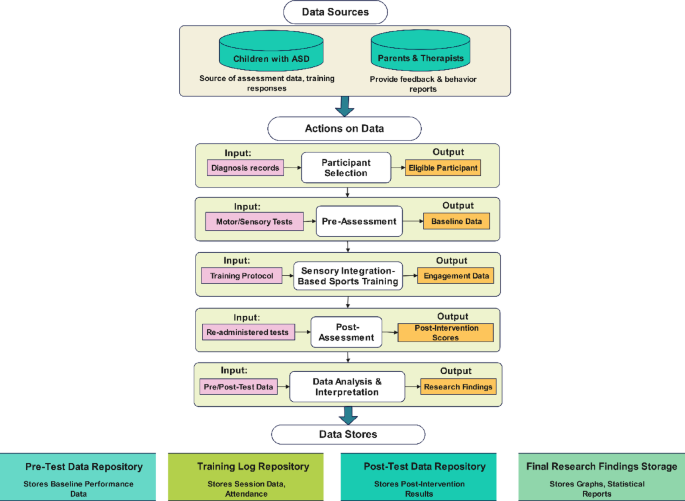
The research design followed a quasi-experimental approach to examine sensory integration-based exercise interventions for sports training effectiveness with children with ASD. The research design applied pre-intervention and post-intervention assessments to track advancements in motor skills, sensory processing functions, and social behaviors of participants. The study separated its participants into two parts: The experimental group gained sensory integration training in sports, while the control group did typical physical exercises without sensory integration components. Researchers employed a mixed-methods approach that combined quantitative assessments, including standard motor skill tests and sensory processing surveys, with qualitative observation methods, including behavior observation and parent and therapist interviews. The research design allowed researchers to understand the complete effects of the intervention on autistic children. The research methodology appears in Fig. 1 through a data flow diagram (DFD).
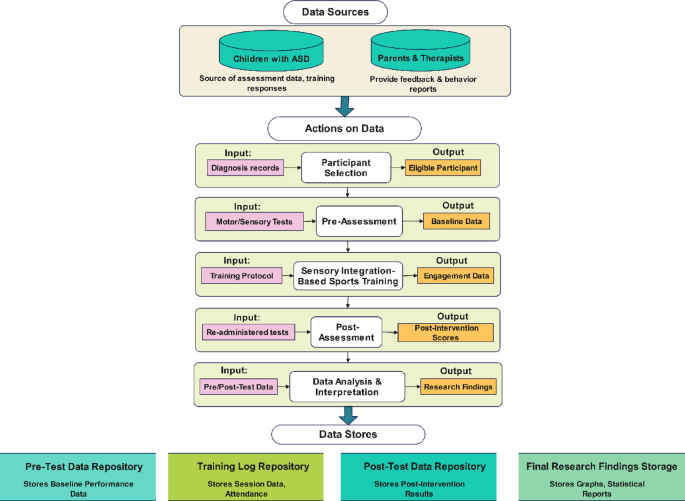
Data Flow Diagram of Research Design.
The research followed a structured, four-phase procedure: participant selection, pre-assessment, intervention implementation, and post-assessment with data analysis. Children aged 6 to 12 years with a formal diagnosis of Autism Spectrum Disorder (ASD) were recruited from three therapy centers and two inclusive schools. Participants were required to demonstrate motor coordination difficulties (scoring at least 1 SD below the mean on the Bruininks-Oseretsky Test of Motor Proficiency [BOT-2]) and sensory processing challenges, as indicated by Sensory Processing Measure (SPM) scores at or below the 30 th percentile.
To ensure cognitive suitability for participation, children with WISC-V scores below 50, as well as those unable to follow simple instructions or complete structured activities, were excluded. Additional exclusion criteria included prior intensive physical therapy within six months, and comorbid neurological conditions (e.g., cerebral palsy, epilepsy) that could compromise motor performance or intervention safety. Children displaying severe behavioral issues, such as aggression or self-harm, were also excluded for ethical and safety considerations.
From an initial pool of 65 screened candidates, 40 children met the inclusion criteria. They were randomly assigned to one of two groups:
-
The experimental group (n = 20) participated in a 12-week sensory integration-based sports training program, involving vestibular activities (e.g., balance beams, trampoline jumps), proprioceptive tasks (e.g., resistance games, obstacle navigation), and tactile exercises (e.g., textured object play, sensory stations), each designed to address individual sensory profiles.
-
The control group (n = 20) engaged in standardized physical education-style routines, such as aerobic games, ball handling, and calisthenics, with no specific sensory integration adaptations. Both groups trained three times per week for 60 min.
Pre- and post-intervention data were collected using the BOT-2 and Social Responsiveness Scale (SRS-2). Weekly behavioral engagement and therapist observations provided qualitative data, which were thematically analyzed to contextualize quantitative outcomes.
The final sample had a mean age of 8.3 years (SD = 1.7) and a gender ratio of 3:1 (male: female), reflecting ASD prevalence. 83% of participants showed SPM scores below the 25 th percentile, and all scored at or below the 20 th percentile on BOT-2, confirming the appropriateness of the intervention target group. Efforts were made to ensure diversity in ethnicity and socioeconomic background, improving the relevance of findings to varied community contexts.
Intervention protocols
The procedure included a 12-week sports training program based on sensory integration, which focused on improving motor skills, sensory processing, and social interaction abilities among ASD children. The physical activities during sessions took place three times per week for sixty minutes while targeting the vestibular, proprioceptive, and tactile systems. The program divided each session into four sections: warm-up, sensory integration exercises, and sports-specific drills before the cool-down session. A 10-minute warm-up with light aerobic activities, including jogging, stretching, and jumping, served as preparation for sensory involvement. Sensory integration activities consisted of 20 min and involved balanced exercises on stability boards, trampoline jumping for the vestibular system resistance training, and tangible object manipulation for proprioception and tactile experiences. The sports-specific training segment included modified soccer drills, basketball dribbling with weighted balls, and obstacle course challenges that enhanced coordination and spatial awareness. Small-team athletic activities promoted collective gameplay and sharing turns, improving students’ capacity to interact with others. Stretching combined with deep-pressure exercises and guided breathing composed the ten-minute cool-down phase, which helped regulate sensory input and lower hyperactive behavior. Standardized assessment instruments were used to monitor participant development during weekly evaluations as part of the study design through BOT-2 and Sensory Profile Questionnaire testing methods. The program introduced customized changes since it needed to establish individualized instruction methods for every student. Location-based trained healthcare professionals supervised the sessions with sports coaches who reported progress to students’ parents for at-home sensory sessions. A new therapeutic approach joined sensory integration protocols with sports organizations to create effective autism treatment, which enhanced motor skills, sensory functionality, and social behavior. Table 1 provides a detailed breakdown of the 12-week sensory integration-based sports training program, including session structure and targeted sensory goals.
Intervention protocols
The program delivered a sensory integration-based 12-week sports training to enhance motor functions, sensory processing, and social relationship abilities of children diagnosed with ASD. The structured session program included activities that lasted for sixty minutes per day and took place three times each week to stimulate the vestibular and proprioceptive, along with the tactile systems of participants. Each training session had four distinct sections, which started with a warm-up, later included sensory integration activities and sports drills, and ended with a cool-down phase. The first ten minutes of the exercise session used light aerobic movements, including jogging, stretching, and jumping, to support sensory involvement. Balance training on stability boards, trampoline jumping, resistance exercises, and tactile interaction with different textured objects were part of the sensory integration phase, which lasted 20 min. Adapted sports drills, including modified soccer skills and basketball ball handling with resistance weights and obstacle course training, were present during the sports-specific training phase, which lasted for 20 min. The games for small teams allowed children to collaborate while practicing turn-taking, thus fostering better social relationships. The ten-minute cooling-down segment included deep pressure exercises, breathing direction, and stretching, which regulated sensory input and minimized hyperactive behaviors. The participants received regular monitoring through standardized assessments containing the BOT-2 and Sensory Profile Questionnaire tests to track their progress. The program followed individual requirements through program adjustments to deliver appropriate treatments. The therapy program received supervision from certified sports coaches and therapists who also delivered progress reports to parents every two weeks to promote home-based sensory practice. The treatment used sensory integration methods and a sports training structure to deliver engaging therapeutic practices that improved motor functions, sensory management, and social interaction among autistic children.
Data collection procedures
Data collection was conducted in three phases: pre-assessment, ongoing monitoring during the intervention, and post-assessment, to evaluate the effects of the sensory integration-based sports training on children with ASD. In the pre-assessment phase, standardized tools were administered one week before the intervention. These included the Bruininks-Oseretsky Test of Motor Proficiency (BOT-2) to assess motor coordination, the Sensory Processing Measure (SPM) to evaluate sensory integration challenges, and the Social Responsiveness Scale (SRS-2) to measure social interaction abilities. In addition, parents completed questionnaires to provide contextual data on their child’s sensory-related behaviors and social functioning in daily life. During the intervention phase, data were collected weekly using a combination of quantitative tracking and qualitative observation methods. Therapists used structured checklists to document behavioral changes, task engagement, and responsiveness to sensory stimuli. They also maintained qualitative field notes on each participant’s adaptability and social participation within the training environment. Attendance was recorded to ensure consistency, and any adjustments made to individual training protocols were documented to track modifications in response to participant needs. In the post-assessment phase, the same standardized tools (BOT-2, SPM, SRS-2) were re-administered to assess progress in motor, sensory, and social domains. Changes were evaluated by comparing pre- and post-intervention scores. Additionally, semi-structured interviews with parents and therapists provided insight into perceived improvements and contextualized the quantitative outcomes. All data were anonymized and securely stored, adhering to ethical guidelines to protect participant confidentiality. Quantitative data were analysed statistically, while qualitative data, derived from therapist notes and parent interviews, were subjected to thematic analysis. The integration of both data types provided a comprehensive understanding of how sensory integration-based sports training influenced developmental outcomes in children with ASD.
Data analysis
Data analysis employed a mixed-methods approach, combining quantitative and qualitative techniques to evaluate the effectiveness of sensory integration-based sports training on motor coordination, sensory processing, and social responsiveness in children with ASD. Quantitative data collected from BOT-2, SPM, and SRS-2 assessments were analyzed using descriptive statistics to summarize baseline and post-intervention scores. Paired sample t-tests were conducted to determine the statistical significance of changes between pre- and post-test scores across motor and social domains. Additionally, Cohen’s d was calculated to estimate the effect size of the intervention, with values interpreted to assess the magnitude of observed changes. Qualitative data, including weekly therapist observations, field notes, and semi-structured interviews with parents, were analyzed thematically. Common patterns in social behavior, engagement, and adaptability were identified and coded using manual qualitative analysis techniques. These findings were then used to triangulate and contextualize the quantitative results, providing a more comprehensive understanding of the intervention’s impact on each child’s development.
Quantitative data analysis
Pre-test and post-test scores from the BOT-2 were compared for motor skill assessment. Each participant’s motor skill score is denoted as \(\:M\), was measured before (\(\:{M}_{pre}\)) and after (\(\:{M}_{post}\)) the intervention. The percentage improvement in motor skills was calculated using:
$$\:Motor\:Improvement\:\left(\%\right)=\left(\frac{{M}_{post}-{M}_{pre}}{{M}_{pre}}\right)\times\:100$$
(1)
.
SPM scores were analyzed for sensory processing. Sensory performance is denoted as \(\:S\), was measured pre- and post-intervention, and the change in sensory responsiveness was determined by:
$$\:\varDelta\:S={S}_{post}-{S}_{pre}$$
(2)
.
where a positive \(\:\varDelta\:S\) indicated improvement in sensory processing. For social interaction analysis, the SRS-2 provided raw scores measuring social engagement. The mean difference between pre-test and post-test scores was calculated as:
$$\:\stackrel{-}{D}=\frac{\sum\:\left({SRS}_{post}-{SRS}_{pre}\right)}{N}$$
(3)
.
where \(\:N\) is the total number of participants. A negative \(\:\stackrel{-}{D}\) indicated improved social responsiveness, as lower SRS-2 scores reflect better social communication. A paired sample t-test was conducted for motor skill, sensory processing, and social interaction scores to determine the statistical significance of observed improvements. The t-statistic was computed as:
$$\:t=\frac{\stackrel{-}{D}}{{s}_{D}/\sqrt{N}}$$
(4)
.
Where \(\:\stackrel{-}{D}\) is the mean difference between pre-test and post-test scores, \(\:{s}_{D}\) is the standard deviation of differences and \(\:N\) is the sample size. A p-value (p < 0.05) indicated a statistically significant difference between pre-test and post-test results. To measure the magnitude of improvement, Cohen’s d effect size was calculated using:
$$\:d=\frac{\stackrel{-}{D}}{{s}_{D}}$$
(5)
.
where values of \(\:d\) were interpreted as 0.2–0.5 (small effect), 0.5–0.8 (moderate effect), and > 0.8 (large effect).
Qualitative data analysis
Observational notes, therapist reports, and parent interviews were analyzed using thematic coding to identify recurring patterns in behavioral improvements, sensory regulation, and social interactions. Thematic clusters were quantified based on frequency and classified into positive responses, neutral responses, and challenges to assess subjective experiences. By integrating quantitative statistical methods and qualitative insights, the analysis provided a multi-dimensional evaluation of the effectiveness of sensory integration-based sports training. A significant increase in motor coordination, sensory adaptation, and social participation confirmed the intervention’s effectiveness, with findings reinforcing the role of sensory-based exercise in rehabilitation programs for autistic children.
Instruments and measurements
The research employed multiple measurement methods, including standardized evaluation tools, observation techniques, and subjective feedback, to assess the success of sports training programs based on sensory integration for ASD children. Measures collected by validated tools assessed motor skill competence, sensory processing ability, and social interaction patterns of the subjects.
The BOT-2 evaluated three motor domains: coordination, balance, fine motor control, and gross motor skills. The test administered percentile ranks and standard scores to enable comparison of motor skills before and after the intervention. The SPM test evaluated sensory processing functions by measuring touch-based, body-positioning, and balance-related responses. The SPM sensory processing assessment generated three categories: typical responses, at-risk performance, and definite dysfunction.
The SRS-2 evaluated social interaction improvements by assessing social awareness, communication abilities, and restricted behavioral patterns. The researchers administered the tool to parents twice to measure social engagement through quantitative results. The behavioral observation checklists monitored participant engagement, adaptability, and responsiveness to sensory stimuli during each session.
Interviews with parents and therapist session reports recorded subjective experiences and changes in behavior that standard tests cannot demonstrate. The team analyzed the qualitative details through themes to understand the intervention’s impact better.
Ethical considerations
The research followed ethical rules to protect participants’ safety and maintain confidentiality and voluntary participant willingness. The investigator received the Institutional Review Board’s (IRB) permission to collect participants before recruitment. Parents and legal guardians provided written informed consent describing the study aims, procedures, risks, and benefits. The research participants learned they could stop their involvement without experiencing adverse effects.
To ensure confidentiality, participant data was protected by applying identification codes instead of personal identifiers. The assessment scores, observational notes, and all other records were stored securely in databases protected by passwords that researchers could access.
The project minimized risks through continuous supervision of trained therapists and sports coaches who adapted the sessions to match the needs of children with sensory sensitivities. Activities followed changes to meet participants’ specific tolerance measures while researchers controlled sensory overload through planned rest time alongside different stimulus options.
The research implemented the Declaration of Helsinki principles to treat all participants ethically. The study team delivered accessible feedback reports that helped parents and guardians understand how their children progressed and received information about the expected advantages of sensory integration exercise treatments.
link







