Understanding pathways for effective interprofessional education: a thematic analysis of medical and nursing students’ insights | BMC Medical Education

16 students from RCSI Bahrain participated in the FGDs and interviews, 62.5% (n = 10) belonging to the School of Medicine (SoM) and 37.5% (n = 6) belonging to School of Nursing and Midwifery (SoNM). A breakdown of the participants is produced in Table 1.
The thematic analysis yielded five overarching themes with associated subthemes from a set of 66 codes (Fig. 1). The relationship exhibited between these themes is one of sequential progression with the initial theme laying the groundwork for the ultimate achievement of the fifth theme.
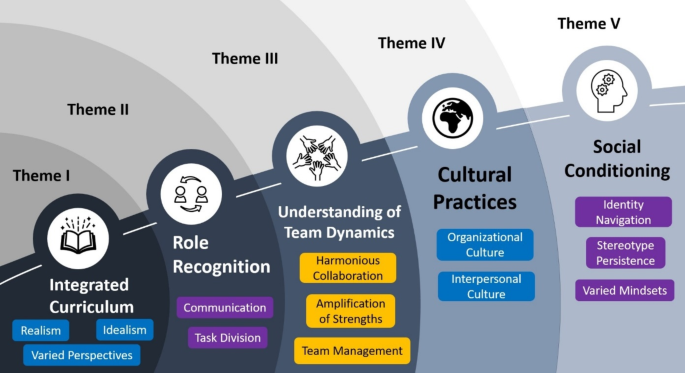
Themes and sub-themes as generated during the thematic analysis
The first theme, ‘integrated curriculum’, is the first step of the staged process that eventually leads to the required prerequisites for effective interprofessional learning, with the fifth theme, ‘social conditioning’, representing the embracement of all attitudes promoting IPE. The first of our five themes is ‘integrated curriculum’, describing the various ways in which IPE and interprofessional collaboration (IPC) can be integrated into the undergraduate medical and nursing curriculums. The second theme, ‘role recognition’, demonstrates participants’ understanding of what each member’s role is in an interprofessional team in a healthcare context. Further, the third theme is ‘understanding of team dynamics’, which is derived from participants’ discussions on aspects of the working processes of an interprofessional team. Additionally, the fourth theme, ‘cultural practices’, represents the organizational and interpersonal cultures in medical and nursing schools, as well as healthcare centers, that affect IPC. The fifth and final theme is ‘social conditioning’, which demonstrates the varied mindsets, attitudes and perceptions regarding interprofessional learning and collaboration.
The themes explain medical and nursing students’ perspectives and attitudes towards as well as experiences with IPE. A more detailed account of these themes and participants’ discussion is produced hereinbelow.
Theme I: integrated curriculum
Interventions in the medical, nursing and health sciences curriculums have been advocated for several decades, with a steering committee of the Institute of Medicine (as it was then known) recommending IPE as a part of the training of healthcare professionals [24]. Following the same line of thought, participants identified interventions into the undergraduate curriculums for medical and nursing students as an effective way of enhancing preparedness for IPC.
Realism
A major chunk of interventions proposed by participants were feasible and practical.
“For the medicine side we have case presentations which are just like there is a patient diagnosed and then present your findings. And for half that is therapeutics and management which should be like involving like a nurse, not just doctors. So why? Why you can’t you combine that? Have doctors diagnosed and then the nursing students would find out what it is.” (Year 2 Medical Student).
Similarly, a majority of participants viewed practical interventions pertaining to IPE as more effective and exciting.
“I think it would be more interesting if we worked together in a clinical setting rather than having lectures together.” (Year 1 Medical Student).
The role of simulation in preparing for IPC was frequently discussed by participants, with many suggesting it as an effective part of the IPE curriculum.
“I feel like one of the best ways [to implement IPE] can be clinical simulation lab, that’s definitely for us as a nursing student we learn the doctor role and the nursing role. But the doctor role is not played by medical students, it’s played by our lecturer, so to be more efficient it can be played by medical students instead.” (Year 4 Nursing Student).
Participants also indicated that social science subjects in the medical and nursing curricula, like professionalism and ethics, are good starting points for IPE.
“Well, honestly, [IPE] could be applied at any stage. …If you get that early on….it is a good way to like get the ball rolling. …So for example and classes that talk about ethics, professionalism between colleagues and patients and nurses.” (Year 3 Medical Student).
Varied perspectives
However, various other opinions were also expressed in this regards, with some participants suggesting that the IPE curriculum must be supplemented with extracurricular socialization of nursing and medical students as well.
“Having both schools together, playing games that are fun, but also learn to communicate with each other. It removes that stigma of medicine students are better than nursing students because it’s like, we’re RCSI students. Especially that there’s no academic aspect to it. It’s just you’re getting to know your fellow students” (Year 5 Medical Student).
Some participants felt that providing opportunities for extracurricular interactions would only serve to further burden students and would thus not be an effective mechanism for rapport building.
“I feel like our curriculum is very strenuous and medical schools as well as nursing school. I think that it would be a difficult part to have interaction together if it is not mandatory. Like I said, it would be difficult to fit in. Because everyone is already their schedules are full. Yeah. It’s very difficult to take time out for anything extra. So it is better to fit within the curriculum instead doing something extra.” (Year 4 Medical Student).
Idealism
Finally, another notable subtheme observed was that of unfeasible, unresourceful IPE interventions being put forward by participants.
“I think having the nurses teaching the medical students would really solve all challenges.” (Year 1 Medical Student).
Theme II: role recognition
One of the many advantageous outcomes of IPE is a better comprehension of the professional roles in a multidisciplinary healthcare team [25]. This was rightly pointed out by participants.
“Well, there’s always kind of like the foundational sort of knowledge. Knowing what each person’s role is. But then also knowing what another person’s role is too. Again, like I said, you have to kind of appreciate the value that each person brings to the table when it comes to healthcare, because each part of like each person’s role is essential. so I think it’s being able to create, appreciate that having the core clinical skills and knowledge, of course and effective communication. Obviously, anytime when you’re working with teams you wanna have effective communication and effective structure.” (Year 4 Medical Student).
The excerpt above, taken from one of the participants’ discussion, sets up both the subthemes when it comes to role comprehension, i.e. communication and task division.
Communication
Participants highlighted the need for communication skills to be part of the IPE curriculum.
We go to the hospital and we don’t really know how to talk to the doctors. I don’t know if I should be friendly with him? Or should I be more professional with him?
This was stressed by participants throughout the FGDs and interviews.
“We have…professionalism classes for how to talk to patients. Yet we have not ever took a single note on how to talk with nurses.” (Year 4 Nursing Student).
T
ask division
Similarly, some participant responses showed that they were not sufficiently aware of roles and task divisions in a multidisciplinary team, confusing the physicians’ role of examining patients with nurses’ role of providing care.
“There’s like, how do you examine patients? Why is that not a collaborative thing? When do…nursing students learn how to like diagnose and how to examine a patient?” (Year 2 Medical Student).
Theme III: understanding of team dynamics
Team dynamics are defined as “the influential interpersonal processes that occur in and between groups over time.” [26] Clearly, these dynamics play an important part in the effectiveness of any multidisciplinary team in providing patient care. Participants identified various facets of team dynamics as conditions for successful IPC.
Harmonious collaboration
One notable dynamic discussed was that of harmonious collaboration through mutual respect and perspective taking.
“I think that it’s vital for everyone’s voice to be heard on the part of the team.” (FY Medical Student).
“I think that this is exactly why understanding the different perspective from each member is very important.” (Year 4 Nursing Student).
“I think also they have to have mutual respect for each other and respect to every team members, ideas, thoughts and plans and like willing to listen to them.” (Year 3 Medical Student).
Similarly, participants expressed that effective communication between members of an interprofessional team was an important factor in its success.
Interviewer: “What makes a healthcare team successful?”
Participant:“Communication. The flow of information. Everyone’s understanding what’s going on because you could communicate all you want to somebody but if they don’t know what you’re saying or they don’t understand what you’re talking about, it’s not going to go anywhere. So make sure that everyone comprehends everything that’s going on.” (Year 5 Medical Student).
A
mplification of strengths
Participants also noted that members of a team must work together in a way that amplifies the total strength of the team.
“Everyone has different qualities, everyone has different strengths, and everyone has their own weaknesses. It is important that in a team we all complement each other. We actually as a team we are complete, we fill in each other’s gaps and that’s what makes teamwork better than individual work.” (Year 4 Medical Student).
T
eam management
Another subtheme that emerged out of participants’ discussions on team dynamics was of team management traits such as shared responsibility and leadership.
“It doesn’t make sense that one person makes a decision or carries the whole responsibility to make such decisions. It is important to, like, have a team to make decisions regarding the patients.” (Year 4 Medical Student).
Theme IV: cultural practices
Professional cultures play a significant role in IPE and IPC, and this is manifested at both the organizational level and also at the interpersonal level through stereotypes and prejudices [27]. In this context, one subtheme that emerged from participants’ discussions was the role of organizational cultures in effective IPE.
O
rganizational culture
Some participants expressed an existing organizational culture of collaboration as being important in successful IPC.
“The environment we’re in should be more about collaboration than competition. Because we’re here for the sake of the patient, not to compete with each other at the cost of the patient’s health.” (Year 1 Nursing Student).
Other participants seemed to view IPC as competition, even if just for the sake of building stronger interpersonal bonds.
“To make them engage more with each other, we should have competitive challenges between them. So, each one would want to prove that he is better than the other one.” (Year 1 Nursing Student).
I
nterpersonal culture
Another important subtheme that emerged was the role of interpersonal cultures as they pertain to the success of an IPE curriculum. Some professional reservations were expressed by nursing students in this context.
“We need to start it off from the foundation of both classes that they have to learn together and live together basically like they need to know how to work together. Cause in the point of view of doctors they don’t understand how important nurses are.” (Year 3 Nursing Student).
A large part of these interpersonal cultures have been discussed in the next theme.
Theme V: social conditioning
Social conditions stand out as pivotal determinants crucial for the success of collaborative efforts in diverse settings [28]. Social conditions can be defined as factors that affect interpersonal relationships [29]. By extension, such conditions also affect the success of IPC in any community, society or profession as a whole.
At various instances throughout the FGDs and interview discussions, participants expressed thoughts and ideas that had to do with social conditions and interpersonal relations. One subtheme that emerged from this was that of identity navigation.
I
dentity navigation
Some nursing students appeared to be hesitant towards engaging in IPE due to an identity threat, i.e. the fear that they would be looked down upon by others in an interprofessional team due to their identity of a nurse.
“We didn’t have the opportunity to work together. If it was, it would be nice and good – uh, beneficial or something. But maybe it won’t be beneficial for other things…….maybe there will be discrimination. Judgements like one of the groups will be thinking we know better than them.” (Year 3 Nursing Student).
In a similar manner, nursing students were seen to have been conditioned into the acceptance of the traditional, stereotypical view of the nursing role.
“As the nurse, you must humble yourself, so [the doctor] doesn’t feel like you’re on the same level.” (Year 1 Nursing Student).
One nursing student exhibited their conditioning into role acceptance by explaining the physician-nurse relationship by giving the analogy of a teacher-student dynamic.
“For example, if I was a student and I had a teacher teaching me, obviously he’s more experienced and has more knowledge than me. So I have to be at a certain level of respect for him because he’s my mentor. … So I have to put myself like not feeling like I’m better than him or anything.” (Year 1 Nursing Student).
S
tereotype persistence
Another subtheme that emerged was the persistence of stereotypes, especially towards the role of nurses in a healthcare team. Participants noted that such stereotypes still exist.
“There’s a lot of misconceptions, definitely. Stereotyping, the misconceptions are just really sad. … I’ve always seen the whole like nursing stereotype, and I didn’t think by the time I would be in med school, it would still be there.” (FY Medical Student).
One participant indicated the existence of stereotypes by recounting an experience.
“For example I know some nursing students who said that when they are with medical students, the medical students don’t look at them or approach them or interact with them at all. That basically the medical students don’t see them as equals. So maybe one challenge might be the students will not interact together due to reasons like this.” (Year 1 Nursing Student).
Participants’ discussion showed that not only did stereotypes exist, but that they also persisted through experiential strengthening.
“I noticed that many nursing students don’t have the ability to speak fluently in English, so there is a language barrier.” (Year 1 Medical Student).
Some judgements were also expressed by participants in regards with the attitudes of physicians towards other members of a healthcare team.
“In the point of view of doctors, they don’t understand how important nurses are.” (Year 3 Nursing Student).
V
aried mindsets
Another associated interpersonal social concept was the display of varied mindsets of participants towards IPE and IPC. Some participants exhibited a very inclusive mindset.
“It builds the RCSI community. Instead of it being a medical school and nursing school, it’s RCSI. So we are all one school.” (Year 5 Medical Student).
Other participants expressed a mindset of flattening the existing hierarchy in healthcare teams.
“What we have noticed as students as well, we have noticed a bias between doctors and nurses in the hospitals. We interact with them every day and we have noticed it. There is an hierarchy like you said. I feel like having an interprofessional learning from the get go when we are students and not doctors will actually help us tackle this bias which we have in the hospital.” (Year 4 Medical Student).
Many participants echoed similar sentiments of the same mindset.
“You as a doctor like you’re equally important, but they’re not below us.” (FY Medical Student).
link





